How to fight against COVID-19
The First Affiliated Hospital, Zhejiang University School of Medicine has treated 104 patients with confirmed COVID-19 in the past 50 days, and their experts wrote real treatment experience when combating the virus night and day, and quickly published this Handbook of COVID-19 Prevention and Treatment.
In order to win this inevitable battle and fight against COVID-19, we must work together and share our experiences around the world.
Part One Prevention and Control Management
I.Isolation Area Management
1 Fever Clinic
1.1 Layout
(1) Healthcare facilities shall set up a relatively independent fever clinic including an
exclusive one-way passage at the entrance of the hospital with a visible sign;
(2) The movement of people shall follow the principle of "three zones and two passag-
es" : a contaminated zone, a potentially contaminated zone and a clean zone provided
and clearly demarcated, and two buffer zones between the contaminated zone and the
potentially contaminated zone;
(3) An independent passage shall be equipped for contaminated items; set up a visual
region for one-way delivery of items from an office area (potentially contaminated zone) to
an isolation ward (contaminated zone);
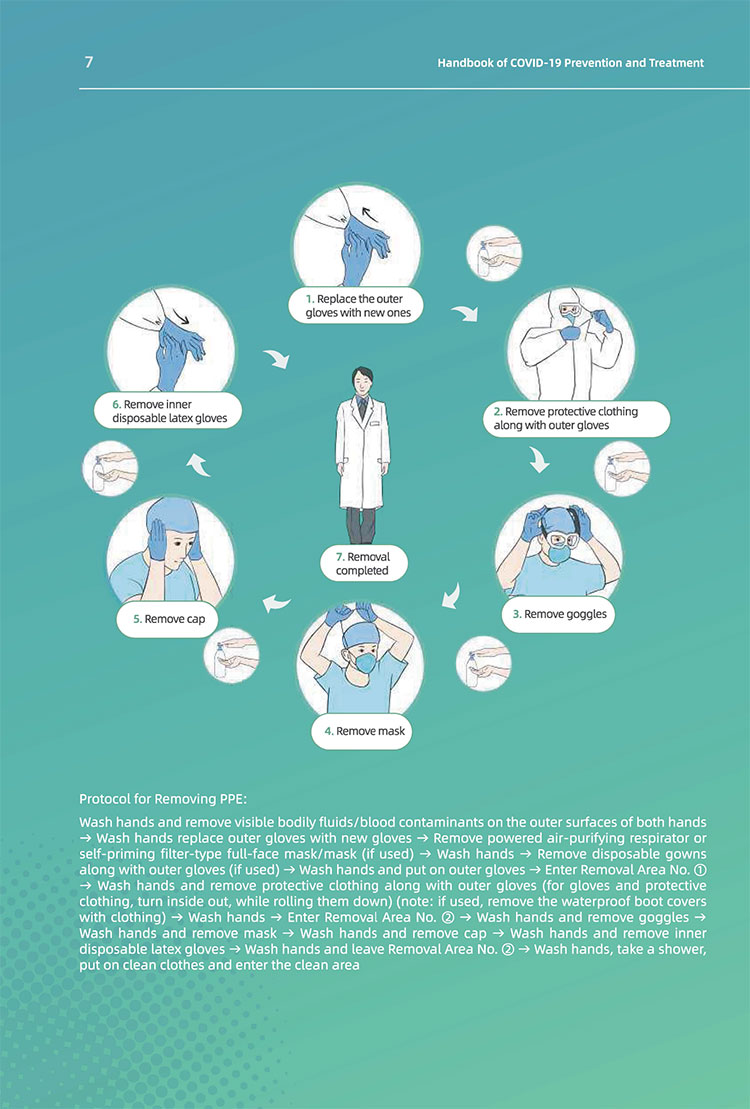
(4) Appropriate procedures shall be standardized for medical personnel to put on and take
off their protective equipment. Make flowcharts of different zones, provide full-length
mirrors and observe the walking routes strictly;
(5) Infection prevention and control technicians shall be assigned to supervise the medical
personnel on putting on and removing protective equipment so as to prevent contamination;
(6) All items in the contaminated zone that have not been disinfected shall not be removed.
1.2 Zone Arrangement
(1) Set up an independent examination room, a laboratory, an observation room, and a
resuscitation room;
(2) Set up a pre-examination and triage area to perform preliminary screening of patients;
(3) Separate diagnosis and treatment zones: those patients with an epidemiological history
and fever and/or respiratory symptoms shall be guided into a suspected COVID-19 patient
zone; those patients with regular fever but no clear epidemiological history shall be guided
into a regular fever patient zone.
1.3 Patient Management
(1) Patients with fevers must wear medical surgical masks;
(2) Only patients are allowed to enter the waiting area in order to avoid overcrowding;
(3) The duration of the patient's visit shall be minimized so as to avoid cross infections;
(4) Educate patients and their families about early identification of symptoms and essential
preventative actions.
1.4 Screening, Admission and Exclusion
{1) All healthcare workers shall fully understand the epidemiological and clinical features of
COVID-19 and screen patients in accordance with the screening criteria below (see Table 1 );
(2) Nucleic acid testing (NAT) shall be conducted on those patients who meet the screening
criteria for suspected patients;
{3) Patients who do not meet the screening criteria above, if they do not have a confirmed
epidemiological history, but cannot be ruled out from having COVID-19 based on their
symptoms, especially through imaging, are recommended for further evaluation and to obtain a
comprehensive diagnosis;
(4) Any patient who tests negative shall be re-tested 24 hours later. If a patient has two negative
NAT results and negative clinical manifestations, then he or she can be ruled out from having
COVID-19 and discharged from the hospital. If those patients cannot be ruled out from having
COVID-19 infections based on their clinical manifestations, they shall be subjected to additional
NAT tests every 24 hours until they are excluded or confirmed;
(5) Those confirmed cases with a positive NAT result shall be admitted and treated collectively
based on the severity of their conditions (the general isolation ward or isolated ICU).
2 Isolation Ward Area
2.1 Scope of Application
The isolation ward area includes an observation ward area, isolation wards, and an
isolation ICU area. The building layout and workflow shall meet the relevant requirements
of the hospital isolation technical regulations. Medical providers with negative pressure
rooms shall implement standardized management in accordance with relevant require-
ments. Strictly limit access to isolation wards.
2.2 Layout
Please refer to fever clinic.
2.3 Ward Requirements
(1) Suspected and confirmed patients shall be separated in different ward areas;
(2) Suspected patients shall be isolated in separated single rooms. Each room shall be
equipped with facilities such as a private bathroom and the patient's activity should be
confined to the isolation ward;
(3) Confirmed patients can be arranged in the same room with bed spacing of not less than
1.2 meters (appx 4 feet). The room shall be equipped with facilities such as a bathroom and
the patient's activity must be confined to the isolation ward.
2.4 Patient Management
(1) Family visits and nursing shall be declined. Patients should be allowed to have their
electronic communication devices to facilitate interactions with loved ones;
(2) Educate patients to help them prevent further spread of C0VID-19, and provide instruc-
tions on how to wear surgical masks, proper handwashing, cough etiquette, medical
observation and home quarantine.
II.Staff Management
1 Workflow Management
(1) Before working in a fever clinic and isolation ward, the staff must undergo strict training
and examinations to ensure that they know how to put on and remove personal protective
equipment. They must pass such examinations before being allowed to work in these
wards.
(2) The staff should be divided into different teams. Each team should be limited to a ma-
ximum of 4 hours of working in an isolation ward. The teams shall work in the isolation
wards (contaminated zones) at different times.
(3) Arrange treatment, examination and disinfection for each team as a group to reduce the
frequency of staff moving in and out of the isolation wards.
(4) Before going off duty, staff must wash themselves and conduct necessary personal hy-
giene regimens to prevent possible infection of their respiratory tracts and mucosa.
2 Health Management
(1) The front-line staff in the isolation areas - including healthcare personnel, medical
technicians and property & logistics personnel - shall live in an isolation accommodation
and shall not go out without permission.
(2) A nutritious diet shall be provided to improve the immunity of medical personnel.
(3) Monitor and record the health status of all staff on the job, and conduct health monitor-
ing for front-line staff, including monitoring body temperature and respiratory symptoms;
help address any psychological and physiological problems that arise with relevant experts.
(4) If the staff have any relevant symptoms such as fever, they shall be isolated immediately
and screened with an NAT.
(5) When the front-line staff including healthcare personnel, medical technicians and property
& logistics personnel finish their work in the isolation area and are returning to normal life,
they shall first be NAT tested for SARS-CoV-2. If negative, they shall be isolated collectively at
a specified area for 14 days before being discharged from medical observation.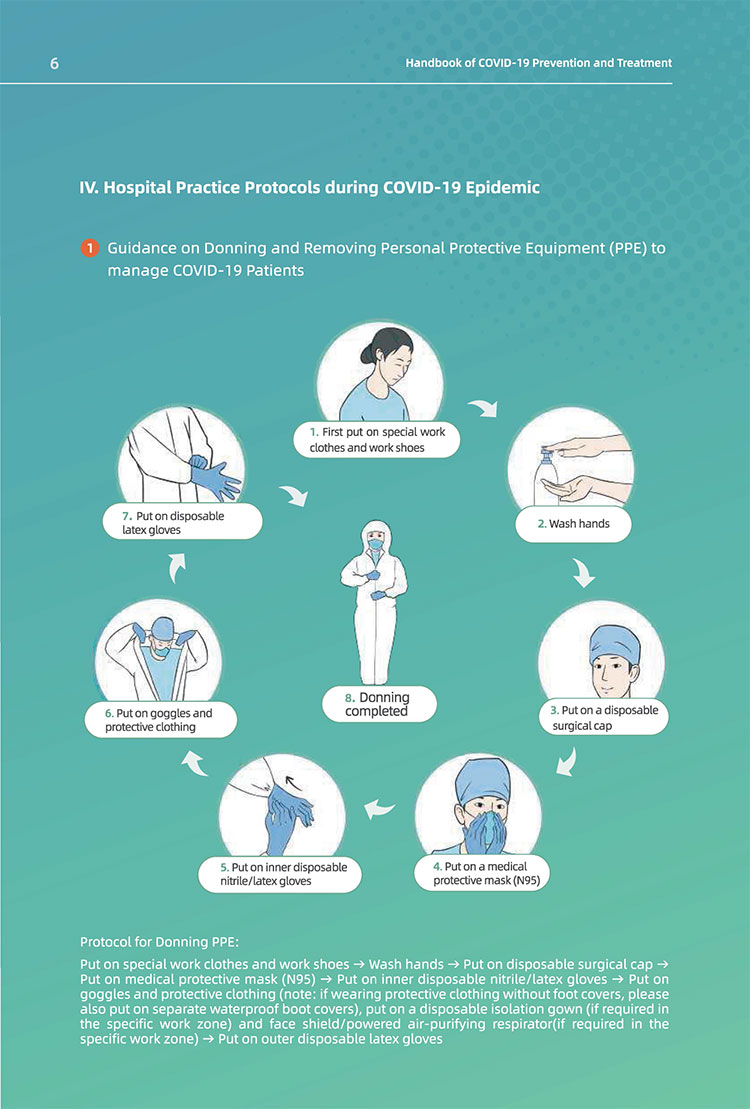
More informations please refers to Alibaba Cloud.